 While many sexual dysfunctions are treated with pelvic floor physical therapy (PFPT), in this post I discuss “dyspareunia”, a common issue I come across with patients. So let’s dive right in. What is Dyspareunia? Dyspareunia is pain before, during, or after sex. Somewhere between 3% to 46% of the population experience it. Some studies say a lifetime prevalence of dyspareunia is 12% in women and 8% in men. In one study from Belgium, about 44% of women and 35% of men reported sexual difficulty. Of that, half of all women and more than half of all men reported that it was distressing, but most did not seek help! There is considerable discrepancy in the numbers across studies. Partially because it’s really hard to talk about, so people are not seeking help. That’s why we are talking about it here. Big issues can often accompany dyspareunia: physical dissatisfaction, poor body image, avoidance of conceiving, and ultimately lack of seeking or maintaining healthy intimate relationships. Why does this happen? There are a host of factors that contribute to painful sex. Here are some main categories: 1. Tight Pelvic Floor Muscles → The pelvic floor muscles are supportive in nature and generally have some amount of activity in them, as explained in Intro to Pelvic Floor. But studies show that people with dyspareunia have higher activation in these muscles. This means that their pelvic floors are working overtime, more than the average person. 2. Dryness → There are a few reasons for dryness, including lack of lubrication, lack of arousal, and lack of prior sexual activity. Some medications including antihistamines are also linked to dryness. In addition, in postmenopausal women, loss of the hormone estrogen can cause thinning of the vaginal tissue, called vaginal atrophy. This causes burning and itching. 3. Musculoskeletal Issues → Simply not being able to sustain a position due to hip tightness or arthritis can be the root cause of dyspareunia. 4. Postpartum Issues → Vaginal childbirth is considered a trauma to the pelvis. After forceps delivery, episiotomy tear, or other injuries, dyspareunia may ensue. 5. Psychosocial issues → Dyspareunia is linked to depression, anxiety, sexual abuse, and fear of sexual abuse. 6. Other Medical Conditions → The following list can either directly or indirectly contribute to dyspareunia. Infections: urinary tract, perivaginal, endometritis, pelvic inflammatory disease
What can I do about it? There is something that can be done for all of the reasons above and PFPT treats many of these causes. Lubrication: For starters, the quickest thing to address is using lubrication to avoid pain from dryness. Many over-the-counter options are available at the pharmacy but a simple organic vegetable oil will do the trick as well. Experiment with what works best for you. Stretching: Understand that just like people can hold tension in their neck or low back, they can also hold tension in their pelvic floor. If overactivity and tightness of the pelvic floor muscles may contribute to your issue, start with this gentle stretch. Take 10 deep belly breaths on each side twice a day. Relaxation and Mindfulness:
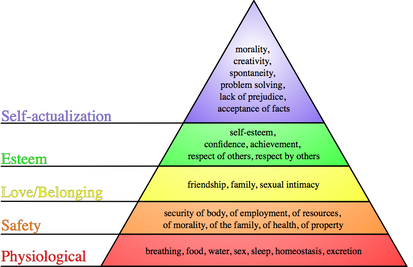
A lot of our muscular tension can come from a psychological cause. I highly recommend getting yourself into a guided meditation practice and regularly taking deep belly breaths. YouTube and Apps such as Headspace and Calm offer plenty of guided meditations. PFPT: A pelvic floor specialist can get you started with dilators, desensitization techniques, soft tissue massage, a home exercise program, and education on muscle retraining. Psychosocial Help: If you have a history of abuse or trauma or experience depression or anxiety about your pain, please seek professional help. A psychologist, counselor, or sex therapist are great people to talk to. Last Thoughts. According to Maslow’s hierarchy, how are we ever going to evolve into the optimal version of humankind if our basic physiological needs are not even met? In Asia, the “Chi” or the “Kundalini” energy are all related to the pelvic floor. Mind you, these are themes that have been spoken about and practiced from nearly the start of these civilizations. So should we care for our pelvic floors in order to fully activate our cerebrum? Something to think about! That’s a wrap for our 3-Part Pelvic Series on “Pooping, Peeing, and Procreation.” I hope you gained something valuable from each of these posts. For those of you who have enjoyed learning from this series, there will be more pelvic blogs soon. For a short time though, let’s switch to some general orthopedics. Our next series will be a 4-Part Series called “Head, Shoulder, Knees, and Toes” where I speak about Headaches, Shoulder Impingement, Patellofemoral Pain Syndrome, and Turf Toe. References: 1. Hendrickx L, Gijs L, Enzlin P. Sexual Difficulties and Associated Sexual Distress in Flanders (Belgium): A Representative Population-Based Survey Study. J Sex Med. 2016; 13:650-668 2. Landry T & Bergeron S. Biopsychosocial Factors Associated with Dyspareunia in a Community Sample of Adolescent Girls. Arch Sex Behav. 2011; 40(5):877-889. 3. McLean L & Brooks K. What Does Electromyography Tell Us About Dyspareunia? Sex Med Rev. 2017; 5:282-294. 4. Messelink B, Benson T, Berghmans B, et al. Standardization of terminology of pelvic floor muscle function and dysfunction; report from the pelvic floor clinical assessment group of the International Continence Society. Neurourol Urodyn. 2005; 24;374-380. 5. Morin M, Carroll M, Bergeron S. Systematic Review of the Effectiveness of Physical Therapy Modalities in Women With Provoked Vestibulodynia. Sex Med Rev. 2017; 5:295-322. 6. Seehusen DA, Baird DC, Bode DV. Dyspareunia in Women. American Family Physician. 2014; 90(7):465-470. 7. Simons J & Carey MP. Prevalence of Sexual Dysfunctions: Results from a Decade of Research. Arch Sex Behav. 2001; 30(2):177–219. 8. When Sex Gives More Pain Than Pleasure. Harvard Women's Health Watch. Harvard Health Publications. 2012; 19(9):1-3. Comments are closed.
|
Dr. GaziWelcome! Learn something of value, solve some of your problems, and feel a whole lot better with Sneha Physical Therapy's blog! Categories |
Sneha Physical Therapy
Copyright 2022 . All Rights Reserved .
Copyright 2022 . All Rights Reserved .



 RSS Feed
RSS Feed